Clinical highlights – September 2022
We are thrilled to inform you about the science of eye tracking. Every month, we will keep you updated on the latest news shared by the scientific community.
The newsletter of this month is related to the relevance of eye tracking in Deep Brain Stimulation (DBS) for Parkinson’s disease (PD).
Enjoy the reading!
The P3Lab team
Deep Brain Stimulation1
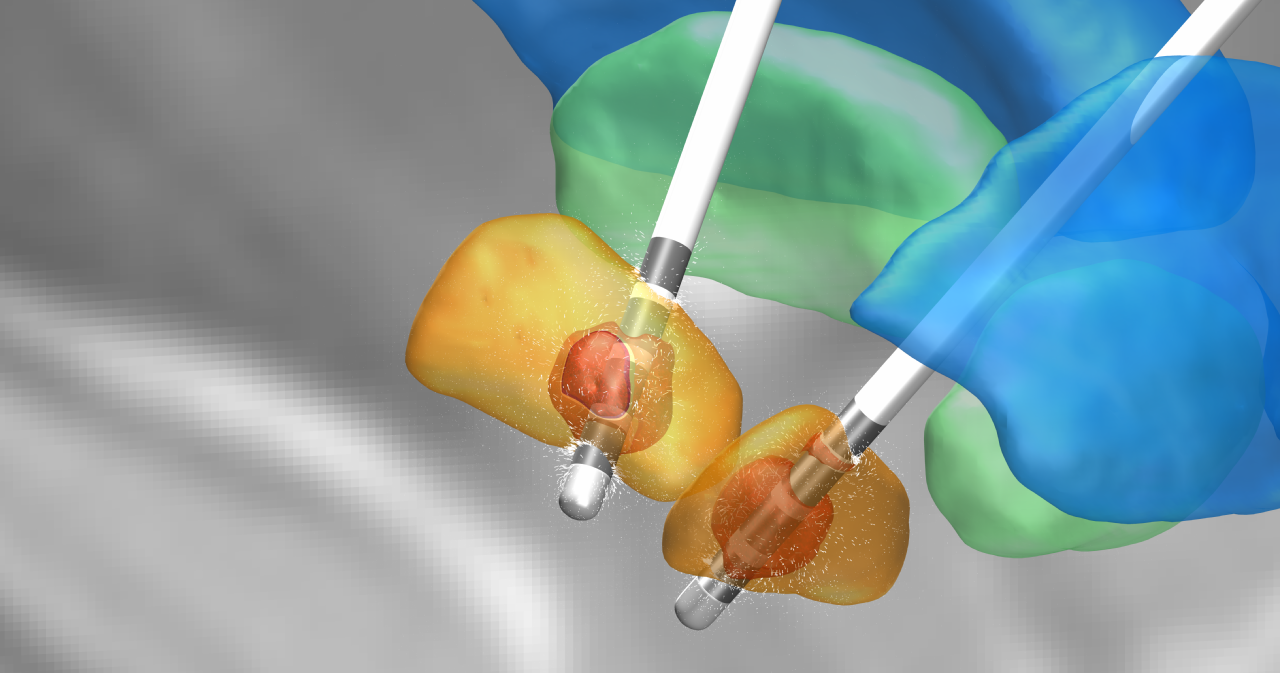
Deep brain stimulation is a neurosurgical procedure that uses implanted electrodes and electrical stimulation to treat movement disorders associated with Parkinson’s disease, essential tremor, dystonia, and other neurological conditions. When successful, DBS interrupts the irregular signals that cause tremors and other movement symptoms through continuous pulses of electric current from the neurostimulator that pass through the leads and into the brain.
The selection of appropriate patients is therefore of particular importance and the individual risk versus benefit ratio has to be carefully assessed.
DBS surgery can help people with Parkinson’s disease improve their symptoms of tremors, stiffness, slowness, and dyskinesias. It can also decrease the dose of medication the patient needs to manage their PD.
Source: Johns Hopkins University
Relevance of eye tracking in neuro-modulation
Eye tracking can provide value during 3 moments in neuromodulation:
- Ahead of the surgery: to better identify target patients based on their clinical prognosis
- Potentially during surgery: to support the most appropriate electrode localization in the operation room
- And finally, after surgery: to refine the patient follow-up in a non-invasive way
Ahead of the surgery
Recent studies have identified antisaccades latency as a predictive biomarker to identify the subpopulation of Parkinson’s patients who will develop freezing of gait, up until 5 years in advance
Antisaccade latency is a predictive marker of the 5-year onset of freezing of gait
… in the case of saccadic latency the pattern is different: surgery produces a transient increase in latency, returning to baseline within three weeks, while subsequent stimulation reduced latency.
During the surgery
Researchers used objective measurement of saccadic latency to compare the effects of surgery and of stimulation.
After the surgery
Recent studies offer the ability to assess the outcomes of basal ganglia stimulation on eye movement behavior in cognitive as well as in motor domains. Understanding the influence of DBS on ocular motor function also leads to analogies to interpret its effects on complex appendicular and axial motor function.
From the clinical perspective such studies provide valuable guidance in efficient programming of stimulation profile leading to optimal motor outcome.
You want to know more?
Our experts have gathered a comprehensive list of scientific literature about the relevance of eye tracking in neuromodulation. Feel free to contact us a request a copy.